
Vitamin E is essential for optimum functioning of many biological systems in animals. It has important functions in the muscular, nervous, circulatory, reproductive and immune system. Vitamin E is also one of the most potent biological antioxidants and a free radical scavenger, functions that are well established and described in the scientific literature. This paper deals with the fundamental role of vitamin E in animal health, its outstanding effect on the immune system and on the prevention of mastitis in dairy cows.
Vitamin E- the effective mastitis fighter
Mastitis is a widespread disease in all major dairying countries despite the considerable progress that has been made in mastitis control over the past 30 years. Milk production potential from the modern dairy cow has soared worldwide: the UK Institute for Animal Health reckons that milk flow rates from the average cow have doubled in the last 60 years.
However, the downside of this improvement is also a 12-fold increase in susceptibility to mastitis over the same period. Other research puts the prevalence of clinical mastitis in modern dairy herds at an average 45 cases per 100 cows. The percentage of subclinical mastitis on average is very much higher. These cases are often unnoticed in the cows themselves and only identified by a very high somatic cell count (SCC) in bulk milk samples. Preventative measures against what has become the most important health problem – one can consider it as a professional disease – of dairy cows include careful hygiene in the milking routine, at drying-off and regular milking equipment maintenance. But often overlooked is the crucial effect of dairy cow nutrition in encouraging a natural resistance to the mastitis-causing microorganisms within the animal metabolism. Reliable trial results for more than two decades have pointed to supplementary vitamin E as the most effective dietary method of reducing the incidence of both clinical and subclinical mastitis.
When we talk about profit loss through mastitis there’s no getting away from the fact that the damage is substantial. For instance, Dutch research in 2008 with input from the Dutch Royal Cattle Syndicate, found an average 25% of even first-calvers in a sample of 173 typical dairy herds were infected with subclinical mastitis in the first 100 days of lactation. The first sign is a substantial increase of the SCC (somatic cell count) in milk and this symptom brings with it a corresponding drop in milk yield. A bulk milk SCC of 250 000/ml can result in a milk yield reduction of more than 100 kg/cow/year and, when the count tops 300 000/ml, more than 250 kg/cow/year are lost. In a herd with low incidence of mastitis bulk tank samples should have less than 150 000 cells/ml. Milk with a SCC of greater than 400 000/ml is not permitted to enter the food chain. The results of Swedish research at the University of Uppsala’s Faculty of Veterinary Medicine indicate – for multiparous cows as well as heifers – that clinical mastitis can cost as much as € 275 and subclinical cases around € 60 per lactation. The same research found milk yields were reduced by 150 l in the case of heifers and an average 450 l for cows. Taking a milk price of 0.35 €/kg this meant a loss of € 52.50 in heifers and € 175.50 in multiparous cows (Table 1).
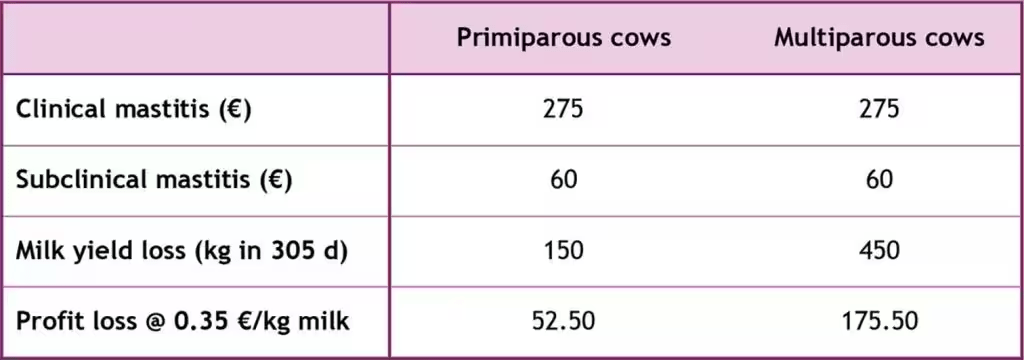
Table 1: The cost of clinical and subclinical mastitis (Nielsen, 2009).
The major problem with mastitis is that it affects much more than milk sales. It is also associated with inflamed and swollen udder quarters – painful to the cow and thus not only a health issue but also an animal welfare problem. Moreover the disease leads to infertility – missed services and longer “empty” days. Sometimes udder quarters are lost to production. In the end, these developments result in increased culling which means the early loss of a good milker, and her genes for future generations in the herd. A survey of the USDA (2007) shows that 23% of cows leaving the herds too early in life are culled because of udder health. After infertility mastitis is the next most important reason for culling on dairy farms.
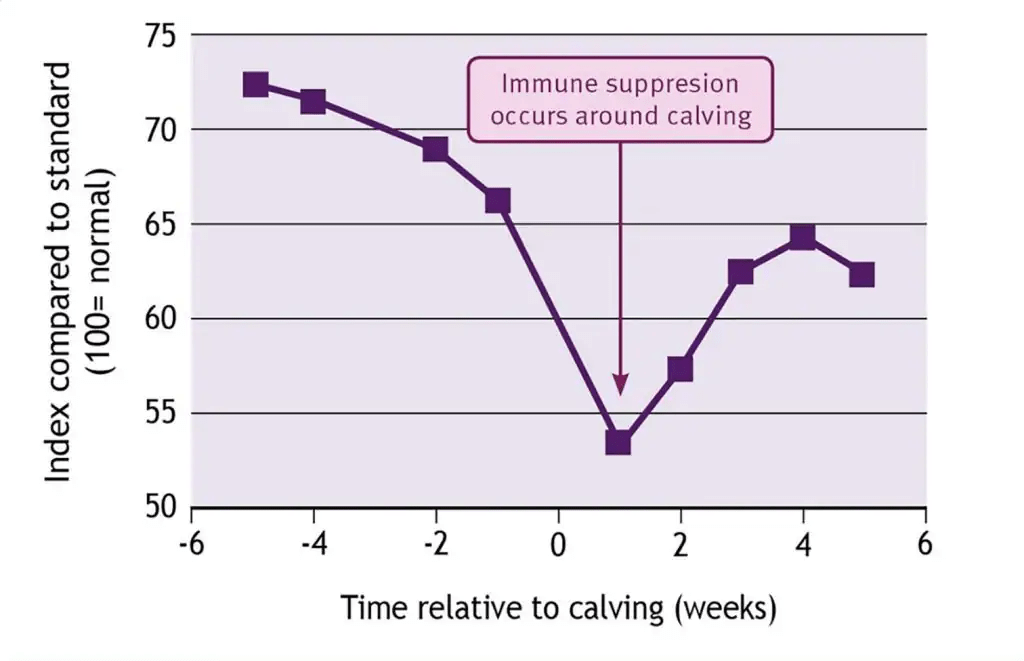
Figure 1: Neutrophil function analysis around calving from 137 Holstein cows (adapted from Kehrli et al., 1994).
There is clear evidence that vitamin E blood levels in dairy cows are always comparatively low at times in the milking cycle when cattle are most susceptible to metabolic disorders. These disorders include the well-known milk fever at calving, but also infections and subsequent diseases. They all occur during the so-called per parturient or transition period that covers the last 10% of the gestation period and the first few weeks into lactation. It is also universally agreed that a component of this stressful time for the cow is a low level of immune response. Figure 1 shows that the neutrophil function is very much depressed around calving, putting cows at greatest risk of developing metabolic and/or infectious diseases after or during calving (Figure 2).
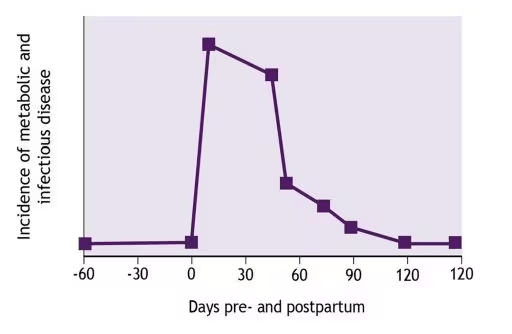
Figure 2: Disease threat is greatest at calving time (Nelson, 1999).
Here plasma vitamin E levels play an important role. Studies have confirmed that plasma vitamin E concentration declines by about 50% in the period around calving and reaches levels that would be diagnostic of chronic deficiency (Figure 3).
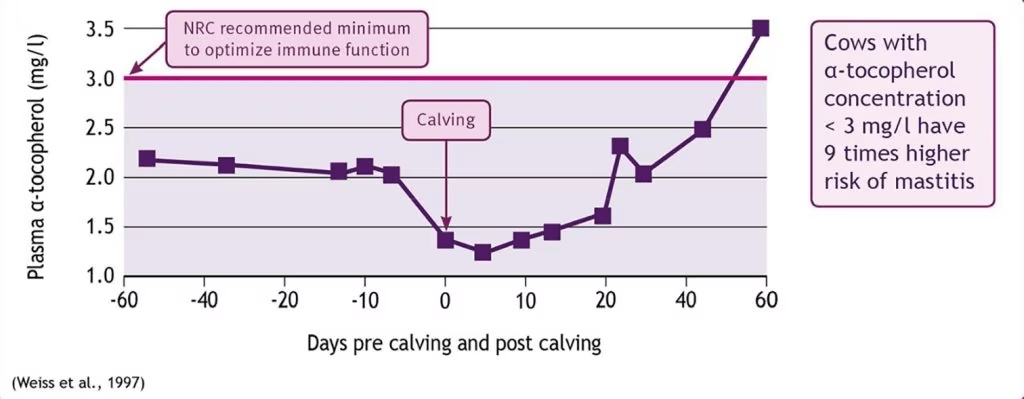
Figure 3: Minimum plasma vitamin E levels recommended by the NRC (2001) to reduce the incidence of mastitis.
The loss is 4 VITAMIN E: A powerful health promoter for dairy cows partly due to sequestration in colostrum. But vitamin E is also consumed at a higher rate as a result of increased immunologic and metabolic stress before calving. An important result is that resistance to disease is weakened. Scientists point out that good resistance relies in part on rapid migration of bacteria-killing neutrophils (immune cells that are the body’s first line of cellular defense) from the blood to the site of infection, for instance to the mammary gland being threatened by invading mastitis-causing microorganisms.
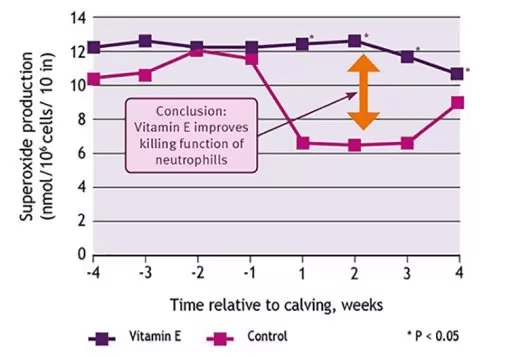
Figure 4: Superoxide production by blood neutrophils from control and vitamin E supplemented dairy cows (adapted from Politis et al., 1995)
This reaction time is slow when vitamin E blood levels are low. It has been clearly demonstrated that cows with low plasma vitamin E levels before calving have a 9 times higher probability of clinical mastitis compared to cows with an acceptable blood level (figure 3). This was recognized by the NRC (National Research Council Committee for Animal Nutrition in the US) in 2001. In its supplementation guidelines it recommends higher dietary vitamin E levels for transition and lactating cows to maintain the minimum plasma vitamin E concentration for optimum immune response. Trials reliably prove that supplementary vitamin E replenishes blood levels with a resultant boost to neutrophil reaction and their subsequent control of those pathogenic “invaders” (Figure 4). While first lactation cows already responded to medium levels of vitamin E, older cows needed higher levels of vitamin E pre and post-partum to reduce the prevalence of mastitis at calving (Figure 5).
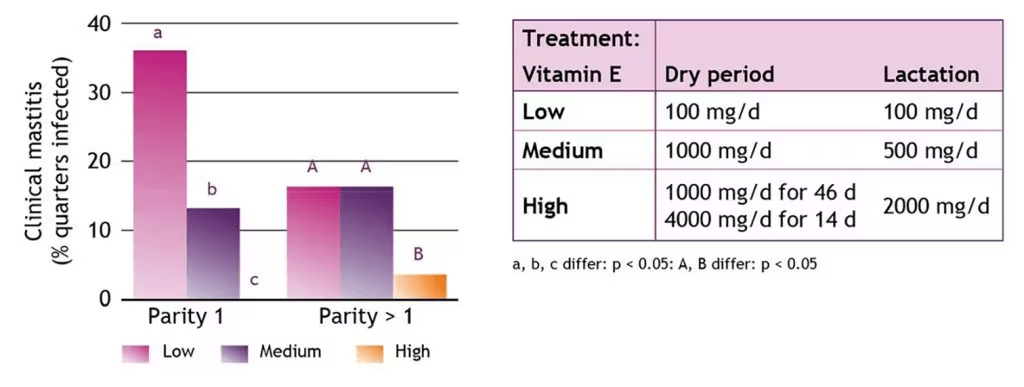
Figure 5: ROVIMIX® E supplementation reduces the prevalence of clinical mastitis of dairy cows at parturition (Weiss et al., 1997).
Figure 6 shows that vitamin E and selenium have a complementary effect on the duration of mastitis. The combination of both reduced the duration of the clinical symptoms of mastitis by 62% compared to the control.
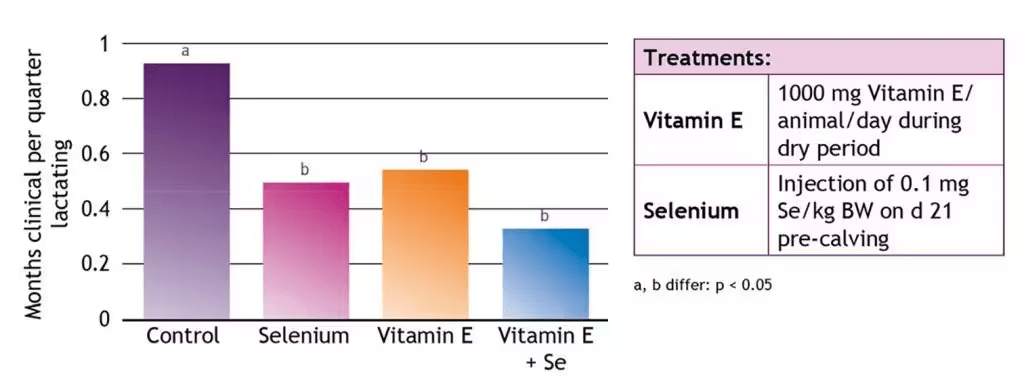
Figure 6: ROVIMIX® E and selenium decreased the duration of clinical mastitis (Smith et al., 1984).
OVN™ Vitamin E supplementation: the answer. Considerable progress has been made in our understanding of vitamin nutrition of dairy cows during the last 15 years. Based on the latest evidence it can be concluded that vitamin E helps to optimize immune function and that it is indispensable for udder health and milk quality. The OVN™ vitamin E recommendations have been compiled based on NRC guidelines, published data and from field trials (Table 2). The response benefit helps to optimize, not only performance and milk quality, but also cow health and welfare. Healthy cows are important for saving costs, thus increasing profits and ensuring longer and more productive milking lifetimes.
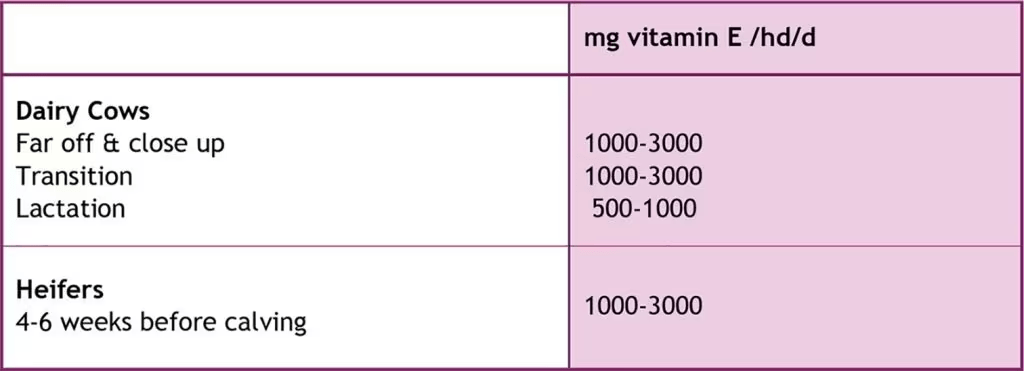
Table 2: OVN™ supplementation guidelines.
